Keep up to date with the latest news and resources from Essendon Physio
It is very important to organise physiotherapy prior to having hip surgery, as prehabilitation (prehab) optimises your recovery post-surgery. For the same reason you complete the preparation of food prior to cooking, it allows for the cooking or in this case hip surgery to run seamlessly.
What is Meniere's Disease, how does it present and does it ever go away? These are the most common questions we get asked and we'd like to help you understand the answers to these and more
Are you experiencing difficulty with opening your mouth, jaw pain while eating hard foods, clicking and locking of the jaw or headaches? There is a one likely culprit and the good news is, we can help.
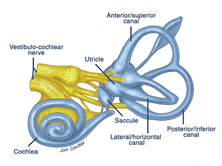
Not sure if your dizziness is coming from your neck, if you have BPPV or Vestibular Neuritis? Let's work through what these conditions are and how we treat them.
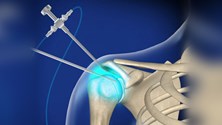
Just about to have a shoulder arthroscopy or commencing your rehab? Let us take you through the procedure, what to expect post surgery and how to plan for your rehabilitation.
Much research has been done to prove the positive effect that Remedial Massage has on our mental health in many different ways, and with these uncertain times it is understandable to not feel completely like yourself, to even feel stressed, anxious or unhappy. Have you tried Remedial Massage with us?
We are passionate about everything Vestibular and given we help so many people with Vestibular hypofunction, Neuritis and Labyrinthitis we've developed a blog outlining what they are in simple to understand language.
Total Knee Replacements are a common knee procedure. Knowing what to do before surgery, what to expect after surgery and how long it will take to recover from the procedure are areas we look forward to exploring with you.
Muscle strains are an extremely common injury; so how do I know that I have a muscle strain and how do I treat a muscle strain? Let's work through these questions with a physiotherapist looking at the latest research.
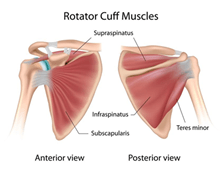
Following rotator cuff surgery, it is important that we move the shoulder to avoid stiffness in the shoulder. This stiffness can progress to a frozen shoulder (adhesive capsulitis) if sufficient movement is not obtained in rehabilitation. So how can physio help and how long does it take to recover from rotator cuff surgery?
Patellofemoral joint (PFJ) dysfunction is a very common condition, but why do people get it and what is the most effective treatment? After a comprehensive assessment to understand what's going wrong, a treatment plan that includes a combination of strengthening exercises as well as some hands on treatment will bring about the best long term results.
Patellofemoral joint (PFJ) dysfunction is a very common condition. But what causes it, how do you treat it and does it ever go away?